-
3D printers
Back
3D printers
Upgrade your classroom with reliable 3D printers used across 10,000+ schools.
Sketch series 3D printers -
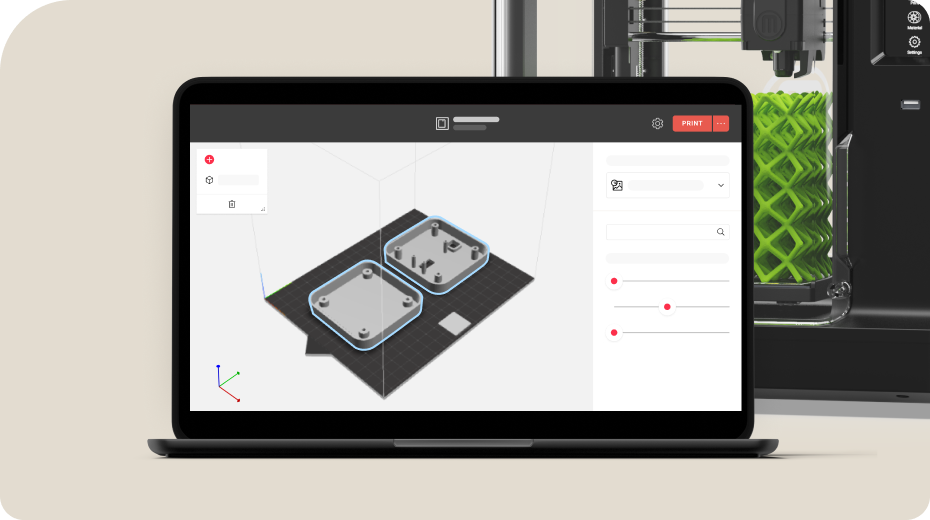
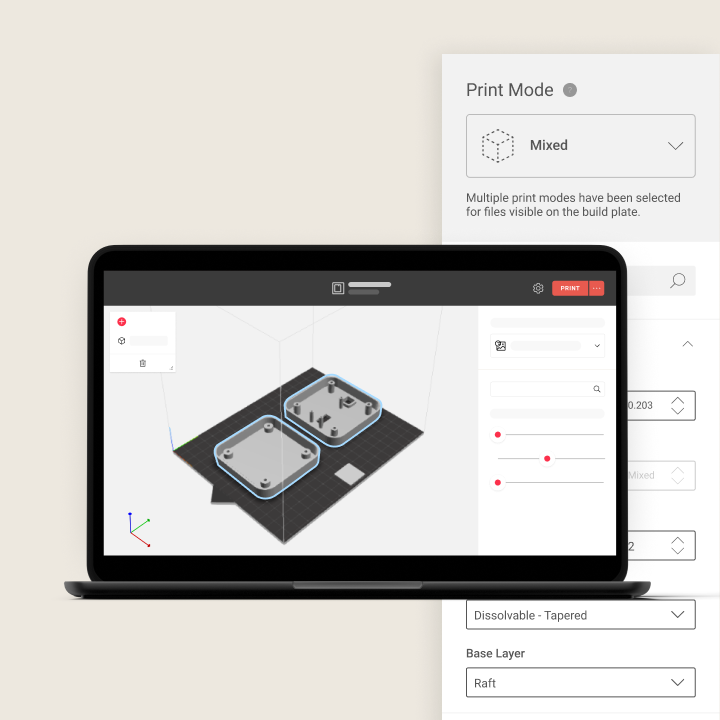
Software
Back
-
Training
Back
Training
Tailored certifications that will help you and your students become experts in 3D printing.
Explore certification -
Resources
Back
Resources
Free access to hundreds of 3D printing lesson plans to help teach a range of subjects.
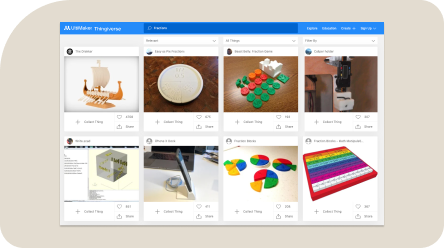
Browse all lesson plans on ThingiverseMakerBot Educator’s Guidebook
Updated for 2023, this guide has become a 3D printing textbook for students and educators.
Thingiverse Education Community
Browse hundreds of 3D printing ideas that help engage students of any subject.
All resources
Get tips and tricks on how to use 3D printing to bring your curriculum to life.
-
Support
Back
Support
Visit our support site for setup videos, how-to guides, FAQs, and technical expertise from our support team.
Support site